Blockchain governance for AI agent payments
Federal agencies are deploying AI agents to process procurement payments autonomously. But existing fraud controls — manual audits, mutable logs, retrospective reviews — were designed for humans, not machines executing hundreds of transactions per minute. The result: $236 billion in improper payments annually, with AI acceleration making the problem worse.
The Solution
Cryptographic Intent Verification (CIV) ensures every AI agent proves its identity cryptographically before initiating any payment — private keys stored in hardware security modules, intent payloads signed and logged immutably.
On-Chain Policy Enforcement (OCPE) evaluates 10 smart-contract rules in real time — from SAM.gov vendor registration to Antideficiency Act budget checks — blocking fraudulent transactions before funds move, not months later during an audit.
What's in the Prototype
Solution Architecture
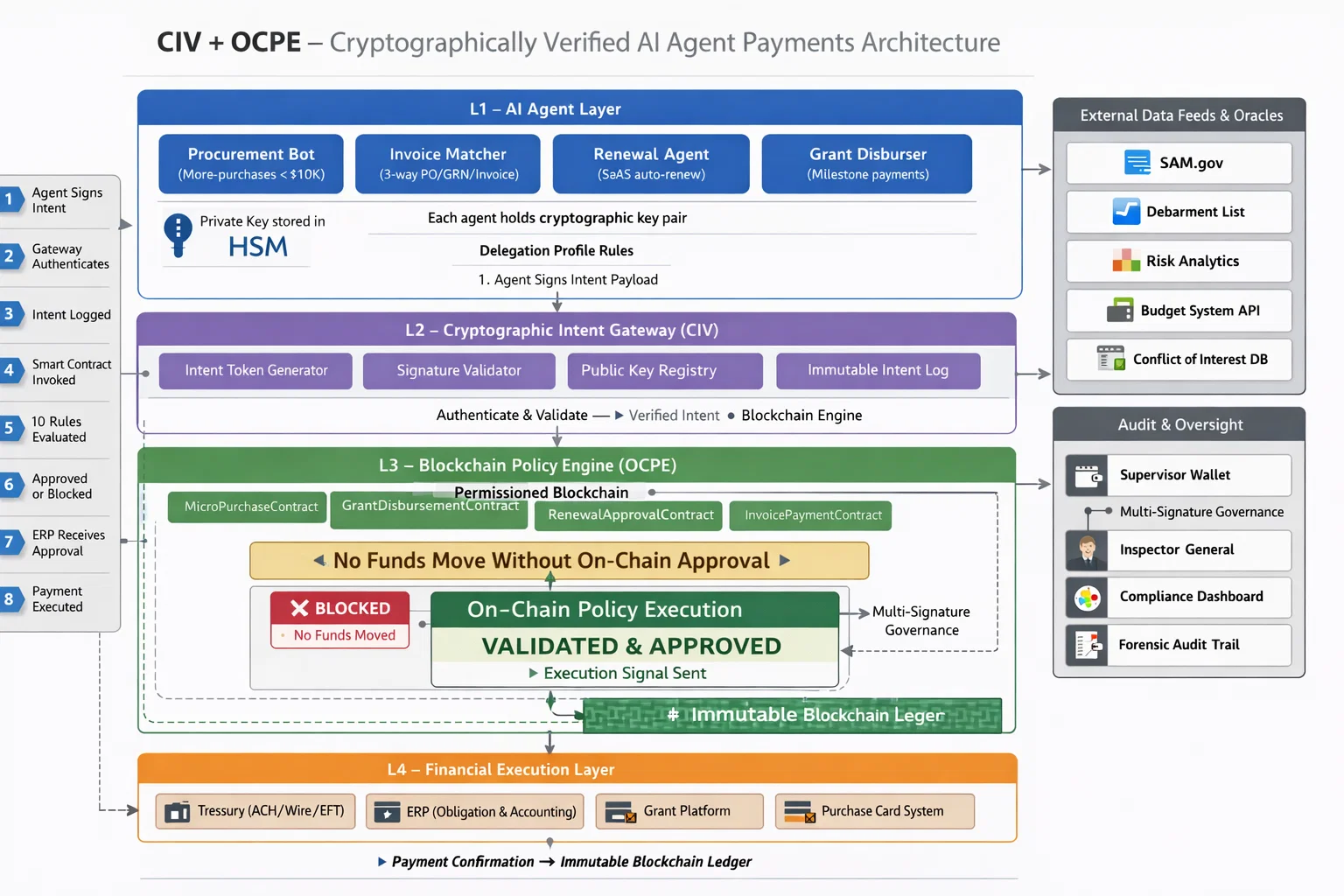
Full Architecture Available on Request
Connect with me to explore the CIV + OCPE architecture in detail — including the working prototype.
Let's Connect →